April 16, 2026
Pelvic floor dysfunction is far more common than most people realize, yet it is rarely discussed openly. Many individuals silently manage symptoms that affect daily comfort, bladder control, confidence, and intimacy. When the pelvic floor muscles are not functioning properly—whether they are too tight, too weak, or poorly coordinated—sexual health is often one of the first areas impacted.
The pelvic floor plays a central role in supporting the bladder, bowel, and reproductive organs. It also contributes directly to sexual sensation, arousal, and orgasm. When dysfunction develops, the effects can extend beyond physical symptoms and into emotional well-being and relationships. Understanding how pelvic floor dysfunction affects sexual health is an important step toward restoring comfort, confidence, and quality of life.
Understanding The Structure And Function Of The Pelvic Floor
The pelvic floor is a group of muscles, ligaments, and connective tissues that form a supportive sling across the base of the pelvis. These muscles help control urination and bowel movements while also stabilizing core movement. Just as importantly, the pelvic floor contributes to sexual sensation and orgasmic response.
When functioning properly, these muscles contract and relax in coordination. This balance supports comfortable intimacy and healthy bladder control. When the pelvic floor becomes weak, overly tight, or uncoordinated, symptoms can begin to surface in subtle or disruptive ways.
Sexual health depends on proper blood flow, nerve signaling, and muscular support. Because the pelvic floor is directly involved in each of these processes, even minor dysfunction can influence physical intimacy. Many people do not initially connect these issues, which delays proper evaluation and treatment.
Recognizing The Causes And Risk Factors Of Pelvic Floor Dysfunction
Pelvic floor dysfunction can develop for many reasons. Pregnancy and childbirth are commonly associated with changes in muscle strength and coordination. Hormonal shifts during menopause may also affect tissue elasticity and muscular control.
Aging naturally reduces muscle tone throughout the body, including the pelvic floor. Surgeries in the pelvic region, chronic coughing, obesity, and repetitive heavy lifting can also contribute. In some cases, prolonged stress and trauma may lead to muscle tension patterns that affect pelvic health.
For men, prostate surgery and age-related changes may lead to similar dysfunction. It is important to recognize that pelvic floor concerns are not limited to women. Anyone can experience challenges related to pelvic floor muscle imbalance.
Understanding the underlying cause helps guide appropriate treatment. The earlier risk factors are addressed, the more effectively long-term sexual health can be preserved.
Identifying The Physical Symptoms That Affect Sexual Health
Physical symptoms of pelvic floor dysfunction vary, but they often include urinary urgency, leakage, constipation, pelvic pressure, or chronic pain. During intimacy, symptoms may present as discomfort, tightness, or reduced sensation.
Pain during intercourse, known as dyspareunia, is frequently associated with overly tight or spasming pelvic floor muscles. When the muscles cannot relax properly, penetration may become uncomfortable or even intolerable. This physical response can create anxiety, which further tightens the muscles and reinforces the cycle.
Weak pelvic floor muscles may lead to decreased sensation or difficulty achieving orgasm. Because these muscles contract rhythmically during climax, reduced strength can diminish intensity. Over time, individuals may notice changes in responsiveness and satisfaction.
These physical experiences can feel confusing or isolating. Many people assume discomfort is normal or unavoidable. In reality, persistent symptoms signal that the pelvic floor may require evaluation and support.
Exploring The Emotional And Psychological Impact Of Pelvic Floor Dysfunction
Sexual health is never purely physical. Emotional connection, confidence, and mental well-being all play a role. When pelvic floor dysfunction interferes with comfort or pleasure, emotional effects often follow.
Individuals may experience embarrassment, frustration, or anxiety related to intimacy. Some begin to avoid sexual activity to prevent discomfort. This avoidance can unintentionally create distance within relationships.
Over time, chronic symptoms may contribute to lowered self-esteem. Concerns about leakage, pain, or performance can create ongoing stress. That stress alone can worsen muscle tension in the pelvic floor, intensifying symptoms.
Open communication and professional guidance are essential. Addressing both the physical and emotional components of pelvic floor dysfunction allows for more complete recovery. Sexual health improves most effectively when both aspects are acknowledged.
Understanding The Clinical Evaluation And Diagnostic Process
Evaluation typically begins with a detailed health history and symptom discussion. Providers may ask about bladder habits, bowel function, pelvic discomfort, and sexual concerns. Honest communication during this stage is critical for accurate assessment.
A physical examination often follows to evaluate muscle tone, strength, and coordination. In some cases, imaging studies or specialized testing may be recommended. Tools such as ultrasound or electromyography can provide insight into how the pelvic floor muscles are functioning.
Assessment may also include questionnaires designed to measure symptom severity and impact on quality of life. These tools help track progress over time and guide treatment decisions. Comprehensive evaluation ensures that therapy is tailored rather than generalized.
When concerns about intimacy are included in the evaluation, providers can better align treatment goals with sexual health outcomes. This integrated approach supports more meaningful results.
Reviewing The Evidence-Based Treatment Options Available
Treatment for pelvic floor dysfunction depends on the underlying issue. If muscles are weak, strengthening exercises such as guided contractions may be recommended. If muscles are tight, relaxation techniques and manual therapy are often prioritized.
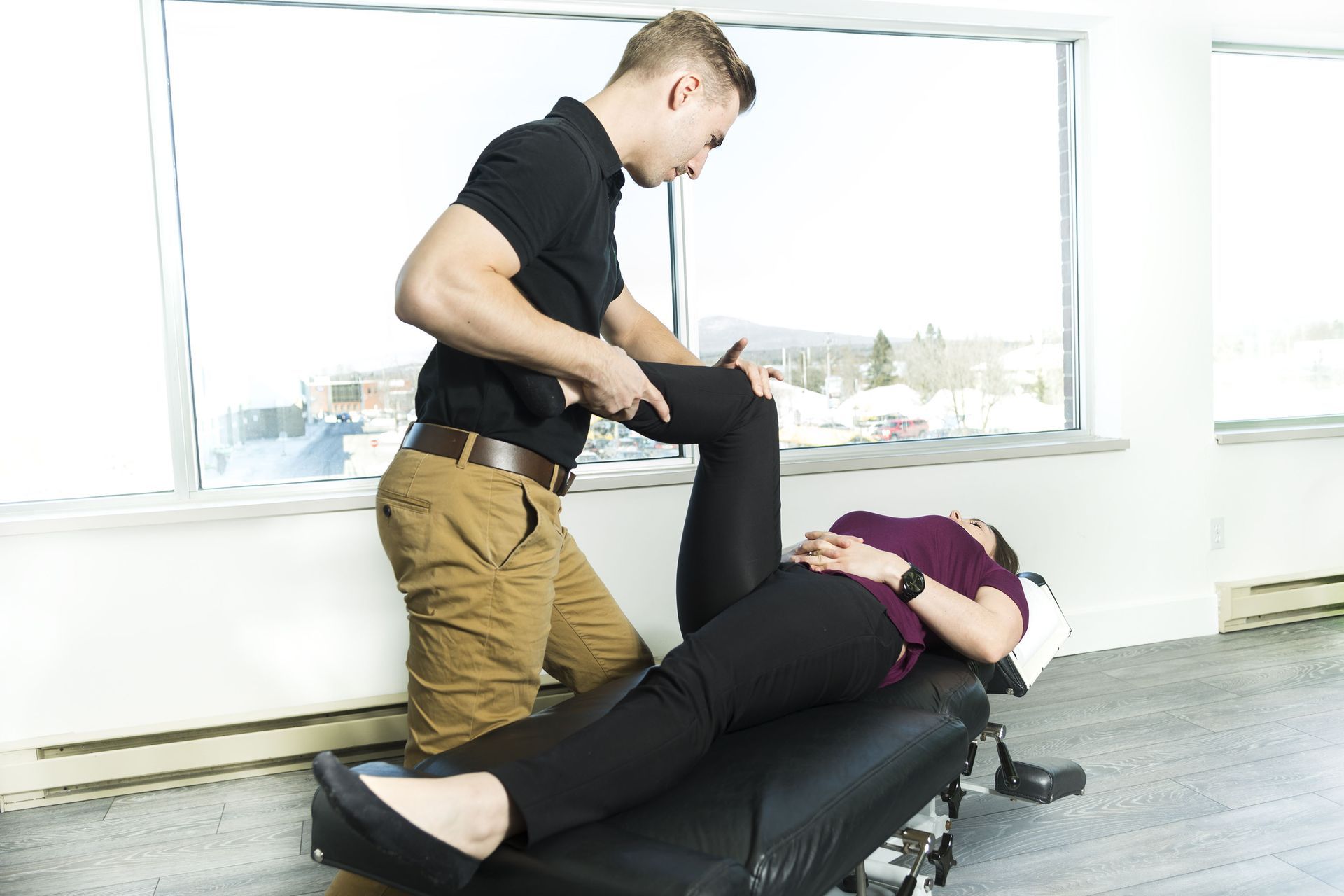
Pelvic floor physical therapy remains one of the most effective interventions. Trained specialists guide patients through exercises that improve coordination, strength, and relaxation. Over time, this targeted therapy supports improved bladder control and sexual comfort.
Technological advances have expanded non-invasive treatment options. According to MDPI, pelvic floor chair therapy using high-intensity focused electromagnetic (HIFEM) stimulation leads to improved urinary continence in 60% to 70% of treated patients. This form of stimulation triggers deep muscle contractions that strengthen and retrain the pelvic floor without surgery or downtime.
Medication may be used in certain cases to address bladder overactivity or hormone-related tissue changes. Surgical intervention is typically reserved for more severe structural concerns. Most individuals benefit from conservative therapy combined with education and lifestyle adjustments.
Strengthening The Connection Between Pelvic Health And Intimacy
Improving pelvic floor function often restores more than bladder control. As muscle coordination improves, many individuals report reduced pain and enhanced sensation during intimacy. Strengthened muscles can increase orgasmic intensity and overall responsiveness.
When discomfort is addressed, anxiety often decreases. This reduction in stress supports better relaxation, which further benefits pelvic floor performance. It becomes a positive cycle rather than a negative one.
Partners may also benefit from education about pelvic health. Open discussion fosters understanding and shared support. When intimacy concerns are approached as a health matter rather than a personal failure, healing becomes more collaborative.
Sexual health is closely tied to physical stability and emotional security. By supporting the pelvic floor, individuals regain both structural strength and confidence.
Emphasizing The Role Of Lifestyle And Preventative Strategies
Preventative care plays an important role in long-term pelvic health. Regular exercise that strengthens the core and pelvic floor helps maintain muscle balance. Avoiding chronic straining during bowel movements reduces unnecessary pressure.
Maintaining a healthy weight can decrease downward stress on pelvic structures. Limiting bladder irritants such as excessive caffeine may also help reduce urinary urgency. Small adjustments can significantly reduce symptom progression.
Education is equally important. Many people are never taught how to properly engage or relax their pelvic muscles. Learning correct technique prevents over-tightening, which is just as problematic as weakness. Proactive care encourages earlier intervention. Addressing minor symptoms before they escalate preserves sexual health and overall comfort.
Pelvic floor dysfunction affects far more than bladder control. It influences intimacy, confidence, and emotional well-being in ways that are often overlooked. When the pelvic floor is not functioning properly, sexual health can be disrupted through pain, reduced sensation, or anxiety surrounding intimacy.
The encouraging reality is that effective treatment options exist. From targeted physical therapy to innovative technologies such as HIFEM stimulation, individuals have access to solutions that restore strength and coordination. When physical care is paired with emotional support and open communication, meaningful improvement is possible.
If you are experiencing symptoms that may be related to pelvic floor dysfunction, seeking guidance can be the first step toward renewed comfort and confidence. To learn more about personalized treatment options, schedule a consultation with Skinn Studio & Wellness Clinic.